Most healthcare organizations have a long history of clinical and/or service quality improvement initiatives. This focus on quality has been stimulated, in part, by regulatory efforts of organizations such as the Joint Commission for the Accreditation of Healthcare Organizations (JCAHO), but healthcare workers' strong mission and commitment have driven its ongoing success.
However, healthcare workers' strong focus on quality improvement may also have a potential disadvantage. Fixating on specific quality improvement measures may lead to an unnecessary narrowing of strategy alternatives. To maintain continuous improvement beyond a certain point, staff members may need to look beyond quality improvement rules and regulations and think creatively about other ways they can affect their patients' satisfaction levels.
Take, for example, nurses' response to patients who press the call button. A typical approach to improving satisfaction in this area is to define a concrete performance standard and measure success according to that standard. For example, the standard might be answering the call button within three minutes. What does this accomplish? The patient uses the call button, a nurse responds. However, because the patient already expected someone to respond in a reasonable amount of time, her satisfaction will not be increased simply because the nurse responds within three minutes. This strategy, while preventing the patient from becoming actively dissatisfied, will not move her from "satisfied" (a "3" on Gallup's scale of 1 to 4) to "very satisfied" (a "4" on a scale of 1 to 4).
What are patients telling the staff when they press the call button? Usually, that they need something and the system failed to provide it without prompting. Thus, the fundamental key to success in this regard is not responding faster, but understanding patient needs better and satisfying them before the need to ask even arises. The ultimate goal is to eliminate the need for the call button by improving need anticipation.
Hospital Performance on Anticipation
Nurses' anticipation of patients' needs has consistently shown the highest level of correlation to overall satisfaction of any question item in Gallup's inpatient satisfaction database. It is also a key factor in improving performance on nearly all other indicators in health delivery settings. Yet great potential exists for improvement on this item.
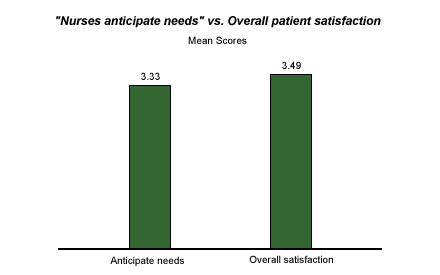
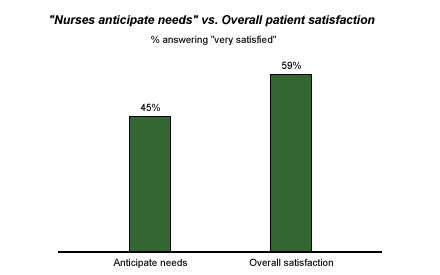
Examples of Successful Anticipation Strategies
It has been my experience that most significant improvement strategies revolve around anticipation of need, as the following examples from Gallup's consulting history illustrate.
Pain Management
Historically, hospitals' approach to pain management has frequently been driven by a fear of addicting the patient to medications. Less was best. Hospital staff interpreted orders to medicate a patient once an hour as no more than once an hour, and only upon patient request -- a reactive strategy. To better handle patient pain management, one ambulatory surgery unit instituted a new process in the recovery room: as soon as a patient awakened, they were asked about the level of pain and their need for pain medication. Patient satisfaction with pain management improved significantly. No change was observed in pain medication use; the improvement was solely based upon implementation of anticipatory behaviors.
Patient Safety
An inpatient unit had an unacceptably high level of patient falls and determined the main cause to be unaided attempts to use the bathroom. One logical response might be an attempt to improve call-button response time. However, most patients who fell had not asked for assistance. The unit implemented a policy of asking each patient at least once an hour if they needed to use the bathroom -- anticipatory behavior. Not only did the number of falls decrease significantly, but patient satisfaction increased significantly.
Key Points
There is a simple key to improving patient service: know your patients and their needs. Do not be trapped in a pattern of always reacting to patient demands without considering how to obviate those needs before the patient recognizes they exist.