The issue of medical errors isn't going away anytime soon. Tens of thousands of patients die each year because of them, and that continues to erode the credibility of the U.S. healthcare system. Consequently, reducing the error rate has become a major public policy focus. But what are the most important factors that need to be addressed?
Policy-makers display unshakable confidence in the power of technology. It's true that advancements in electronic medical records and new pharmacy information systems have benefited patients immensely. Many hospitals have also focused on processes. Physicians' orders for dosage, for example, have been standardized to require that all dose quantities less than one be written with a lead zero (that is, 0.34 g, not .34 g). Patients being prepped for surgery are now typically written on with a marker to fully ensure surgeons identify the correct locations for procedures.
But the efficacy of technological solutions and policy changes relies on whether people properly implement them. Nurses have been identified as a key connecting point through which systems, patients, and physicians work together to identify and prevent potential medical errors. They represent the key "people factor" in controlling healthcare quality. Some think the solution is as simple as increasing the number of nurses in a unit, assuming more bodies will allow for greater quality control. That's probably true to an extent, but Gallup has found that the level of engagement of a facility's existing nursing staff should be the first priority.
Nurse Engagement Reduces Mortality
Using standardized mortality and complication indexes, Gallup studied outcomes at more than 200 hospitals using staffing and other variables, including the level of nurse engagement. A regression analysis of the relationships in the data identified nurse engagement as a key factor.
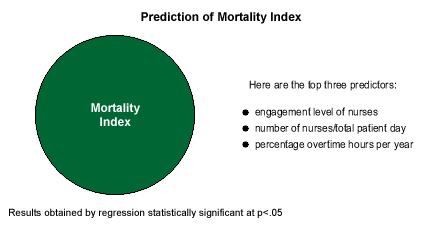
Obviously, the most serious indicator of medical quality is the rate of patient deaths across hospitals. The number of nurses was found to affect this; the ratio of the number of nurses to total patient days was the second-most important factor. The third-most important factor was the percentage of overtime hours per year. Overtime can be a function of understaffing, as vacant positions have to be covered. Too often the result is that tired nurses make mistakes and are unable to function effectively as the key quality control checkpoint that they are.
But the key finding here is that nurse engagement is the No. 1 predictor of mortality variation across hospitals. The commitment and emotional involvement of the nurses on staff is even more important than their numbers.
Engagement Also a Factor in Preventing Complications
The complication index is a more frequent indicator of quality at healthcare facilities. Complications in the form of infections encountered increase patient suffering and the cost of providing care. Reduction in unnecessary complications, as measured by adjusted complication rates across institutions, has always been a key quality goal.
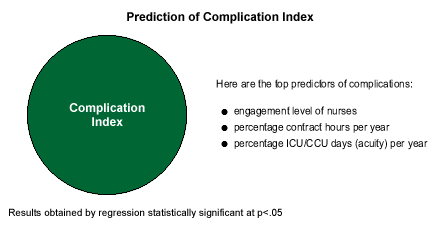
The major variables involved in the complication rate are more complex than those affecting mortality rates. Obviously, the sicker the patient, the more likely complications are to occur. The acuity of patients' conditions, as measured by the percentage of ICU/CCU days per year was the third-strongest predictor of complication variation.
The staffing level again plays a role, this time as measured by the percentage of contract nursing hours per year. Contract nursing hours are high when permanent staff members are unavailable to cover fluctuations in patient volume, and when the facility is unable to fill vacancies. But high complication rates in such facilities shouldn't be simply be attributed to poorer skills among contract nurses. Healthcare quality is a team-dependent variable. Contract nurses may simply have not been as well integrated into the healthcare team due to their transitory natures, or be as familiar with the provider's systems and policies.
Regardless, as it did for mortality rates, nursing engagement emerges as even more important than patient acuity or nursing staff size in explaining the variation in complication rates across hospitals.
Nurse Engagement: No. 1 Quality Priority
In any hospital's effort to improve healthcare quality, the most basic consideration is people -- and particularly nurses -- rather than technology. And within that consideration, the most basic variable is the staff's level of engagement. Certainly, inadequate numbers and broken systems have an effect -- but they do so by lowering staff engagement. For most hospitals today, the engagement level of nurses has the strongest impact on complication and mortality rates.
Are your nurses loyal and psychologically committed to the organization and their jobs? Are nursing managers selected for their management talent rather than just patient care skills? Do nursing staff members have all their performance-related workplace needs met? If hospital administrators can't answer 'yes' with conviction to all of these questions, their patient care quality is at risk.