Story Highlights
- High rates of chronic conditions make U.S. adults vulnerable to COVID-19
- 17% of Americans aged 80+ are at risk of severe illness if infected
- West Virginia has the highest risk level of any state population
WASHINGTON, D.C. -- Over 11 million U.S. adults are at severe risk of critical illness or death if infected with COVID-19. This is based on a special analysis of Gallup National Health and Well-Being Index data examining rates of chronic conditions believed to be key risk factors in addition to smoking rates and population age distribution.
| Total people | Percentage with at least one condition | Percentage at severe risk | Total people at severe risk | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| # | % | % | # | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Age group | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| 18-29 | 53,657,553 | 6.63 | 0.55 | 296,656 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| 30-39 | 42,518,642 | 13.60 | 1.14 | 483,969 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| 40-49 | 40,909,501 | 27.44 | 2.55 | 1,041,192 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| 50-59 | 43,310,372 | 45.05 | 4.80 | 2,080,565 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| 60-69 | 36,150,682 | 61.15 | 7.34 | 2,654,195 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| 70-79 | 20,706,539 | 75.14 | 12.36 | 2,559,528 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| 80+ | 12,122,561 | 78.98 | 16.72 | 2,026,659 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| U.S. adults | 249,375,850 | 11,142,765 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Note: Figures for "Total people at severe risk" may not calculate perfectly because percentages in the table are rounded to two decimal places. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Gallup National Health and Well-Being Index | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
This analysis is not meant to estimate the number of Americans who are at risk of infection, but rather the total number of adults who would have a very high chance of becoming critically ill or dying if 100% of the U.S. population were to become infected with COVID-19. The analysis equally weights age with a composite variable based on respondents' reports that they have high blood pressure, diabetes, a history of heart attack(s) or cancer, in addition to smoking. In other words, the calculations treat age and health status as equal and independent mortality risk factors. (See the Survey Methods section for a detailed description of the methodology.)
The Centers for Disease Control and Prevention has listed age as a major risk factor for experiencing critical illness associated with COVID-19, particularly at age 65 and older. Older adults have a harder time resisting infection as the white blood cells needed to identify and eliminate infections decline in number and efficiency. Risk clearly exists among younger adults as well, although at significantly lower levels.
Several chronic conditions are also known risk factors. Based on an analysis by the Chinese Center for Disease Control and Prevention of COVID-19 in China, as of Feb. 11, 2020, patients who reported no underlying medical conditions had an overall case fatality of 0.9% -- compared with 10.5% for those with cardiovascular disease, 7% for those with diabetes, and 6% each for those with chronic respiratory disease, hypertension or cancer. Smoking and vaping, though not yet carefully studied, are also increasingly assumed to be behavioral risk factors of serious COVID-19 infection due to the respiratory nature of the disease and the manner in which smoking suppresses immune function in the lungs and causes inflammation.
Gallup's National Health and Well-Being Index data are based on over 125,000 completed surveys with randomly selected U.S. adults between January 2018 and August 2019. Age-based mortality rates are based on available published data examining COVID-19 death rates in China and Italy and extrapolated to the U.S. population.
The estimates of people at high risk of becoming critically ill represent expected mortality counts upon 100% infection for those aged 50 and older, but less so for those aged 18 to 49. For example, 0.6% of those aged 18 to 29 in the U.S. -- about 300,000 young adults -- are at severe risk of serious illness or death. In China and Italy (PDF download), only about 0.05% of those in the 20-29 age group have died upon infection, less than one-tenth of this rate. In the case of younger infected persons, therefore, serious illness and hospitalization appears to be a more likely outcome than death based on currently available data.
West Virginia Residents Carry Highest Risk for Severe Reaction to COVID-19
A special analysis at the state level has also been carried out to assess the risk of severe reaction to a novel coronavirus infection. West Virginia was the 50th state to confirm a case of COVID-19 and had just 16 residents who tested positive as of March 23 -- the lowest number in the nation, at the time.
But, West Virginia also has the second-highest percentage of adult residents (48%) with at least one chronic COVID-19 risk factor, and has the third-highest percentage of residents aged 55 and older -- making it the state with the highest risk of severe illness upon infection. West Virginia also has the fourth-highest smoking rate in the U.S., at 17.6%. So, if the outbreak were to begin to take hold and spread widely throughout the state, residents would be expected to be particularly vulnerable to the ill effects of infection.
Alabama, Mississippi, South Carolina and Arkansas round out the top five states with residents most at risk if the COVID-19 outbreak were to spread widely throughout the states.
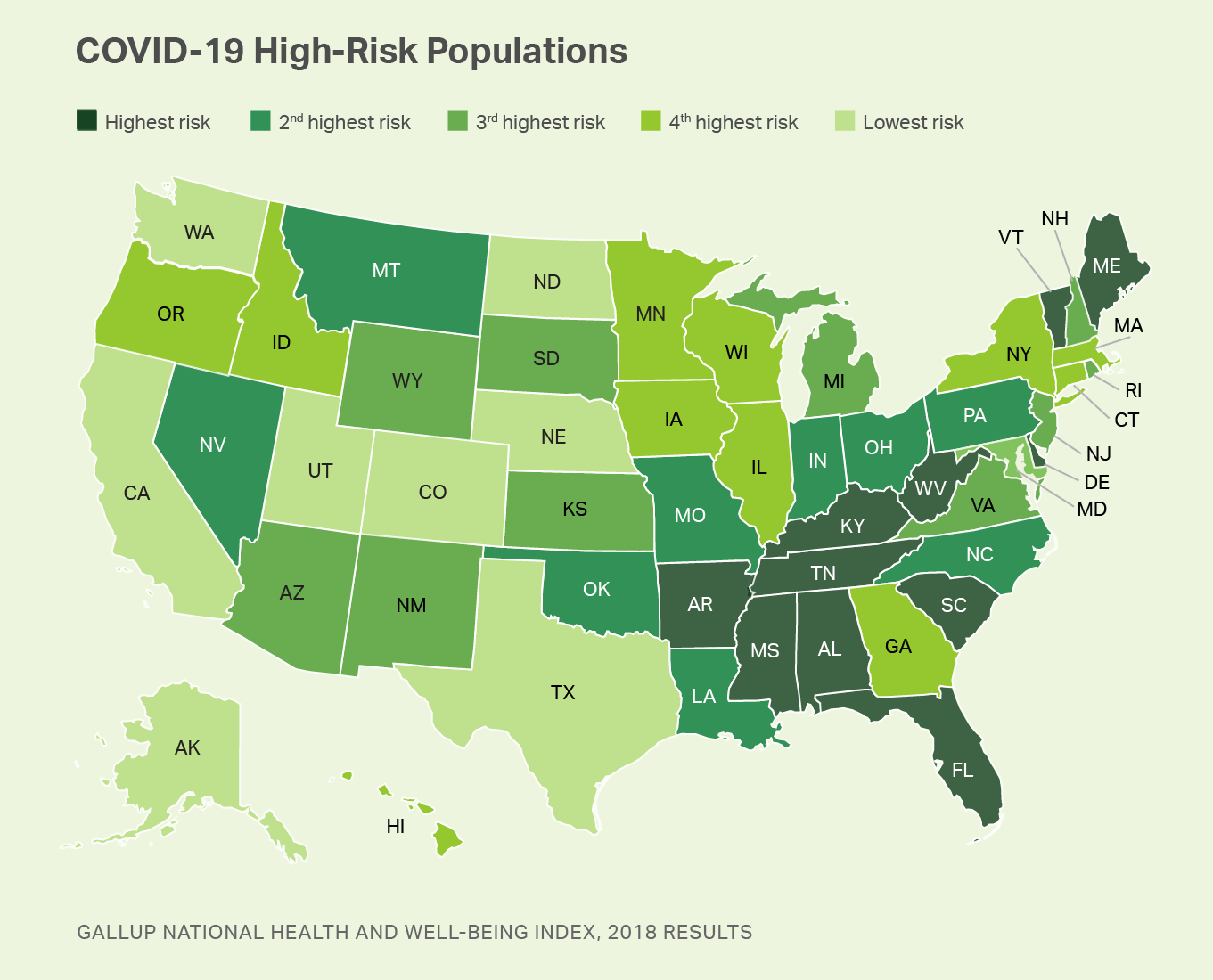
Utah, Alaska, Colorado, California and North Dakota have the lowest risk of severe illness among their respective residencies. It should be noted that even in these states, however, the hospitalization and mortality rates will be very substantial if infection becomes significantly widespread. California had over 2,500 confirmed cases and 50 deaths as of March 24.
Click here to access state-level data on COVID-19 risk factors (file download).
Implications
The role of age as a risk factor independent of the chronic conditions that rise in prevalence with aging is unclear, but available evidence strongly suggests that age alone is its own factor.
In Italy, for example, of the 5,019 deaths due to COVID-19 as of March 23, only 53 occurred in patients younger than 50, according to the COVID-19 Task Force of the Department of Infectious Diseases and the Higher Institute of Health. This indicates that Italian adults aged 50 and older are about 94 times more likely to die from the virus compared with their younger counterparts.
Among chronic conditions, however, no such level of disparity exists anywhere in the world. In the U.S., those aged 50 and older are, on average, about four times more likely to currently have high blood pressure or diabetes and are about nine times more likely to have suffered a heart attack compared with those younger than 50. As such, even in a country such as Italy with a disproportionately older population -- its median age of 47 is about 10 years older than what is found in the U.S. or China -- such considerable differences in death rates indicate the substantial importance of age alone in determining COVID-19-related mortality rates.
The percentage of the U.S. population that will ultimately become infected with COVID-19 within 12 to 18 months from now -- the time frame currently assumed for the approval and mass distribution of a working vaccine -- is unknown. It will depend in part on the success of social distancing and self-isolation in curbing its spread, as well as the frequency and strength of outbreak recurrences. Individual populations within the U.S. will also suffer varying rates of infection based on how densely populated any given area is. In New York, for example, Gov. Andrew Cuomo has estimated that 40% to 80% of the population will ultimately be infected with novel coronavirus. Nationally, if 10% of the adult population becomes infected -- about 25 million people -- then deaths in excess of 1 million would be possible.
What is also undetermined is how closely the infection statistics found in China and Italy will generalize to the rest of the world and to the U.S. in particular. In the U.S., for example, a much higher percentage of young adults appear to be in need of hospitalization for COVID-19 complications than reported elsewhere, which could indicate that a higher-than-expected mortality rate could ultimately be realized.
Learn more about how the Gallup National Health and Well-Being Index works.