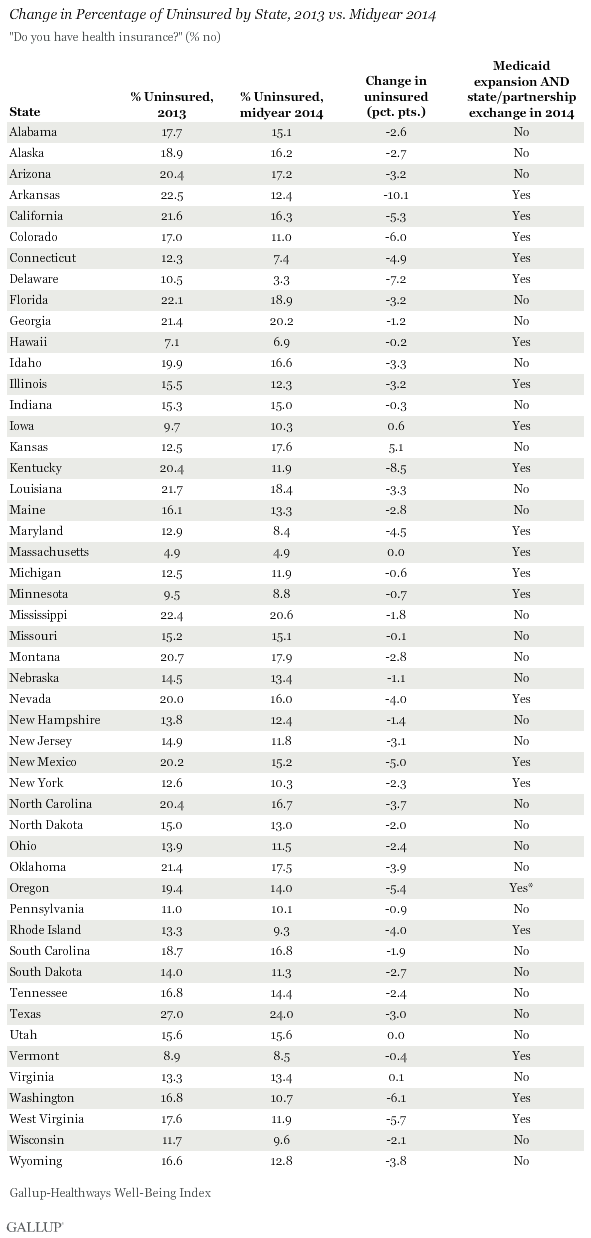
WASHINGTON, D.C. -- Arkansas and Kentucky lead all other states in the sharpest reductions in their uninsured rate among adult residents since the healthcare law's requirement to have insurance took effect at the beginning of the year. Delaware, Washington, and Colorado round out the top five. All 10 states that report the largest declines in uninsured rates expanded Medicaid and established a state-based marketplace exchange or state-federal partnership.
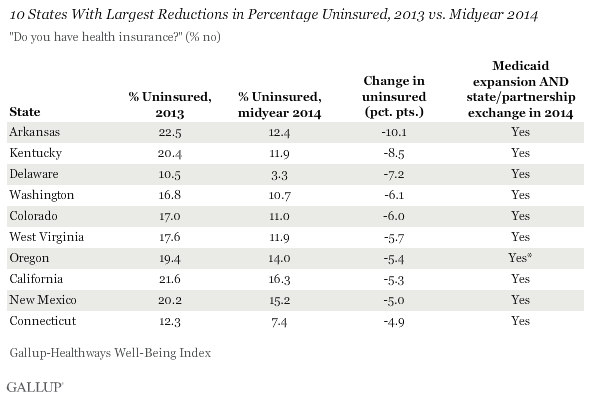
As Gallup previously reported, the states that chose to expand Medicaid and set up their own health exchanges had a lower uninsured rate to begin with: 16.1% compared with 18.7% for the remaining states -- a difference of 2.6 percentage points. The already notable gap between the two groups of states widened through the first quarter to 4.3 points, as states that have implemented these core mechanisms of the Affordable Care Act reduced their uninsured rates three times more than states that did not implement these core mechanisms.
These data, collected as part of the Gallup-Healthways Well-Being Index, are based on respondents' self-reports of health insurance status based on the question, "Do you have health insurance coverage?"
Uninsured Rates Continue to Drop More in States Embracing Multiple Parts of Health Law
The uninsured rate in the states that have chosen to expand Medicaid and set up their own state exchange in the health insurance marketplace has declined significantly more in the first half of 2014 than in the remaining states that have not done so. The uninsured rate declined 4.0 points in the 21 states that have implemented both of these measures, compared with a 2.2-point drop across the 29 states that have implemented only one or neither of these actions.
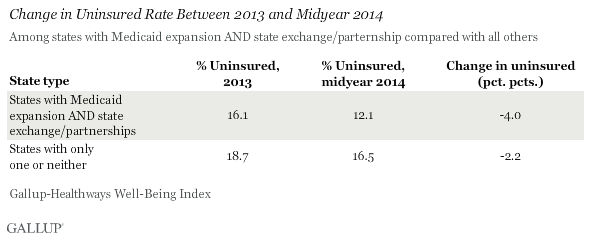
Some states have chosen to implement state-federal "partnership" exchanges, where states run certain functions and make key decisions based on local market and demographic conditions. For the purposes of this analysis, these partnerships are included with the state exchanges. New Hampshire, which manages a state-based exchange but has only recently voted to expand Medicaid, is not included, as its eligible residents were not privy to expanded Medicaid through the first six months of 2014. Four states -- North Dakota, New Jersey, Ohio, and Arizona -- have decided to expand Medicaid without also administering a state-based exchange or partnership, while several others continue to debate its expansion. The District of Columbia, which has expanded Medicaid and has implemented a locally managed exchange, is not included in this analysis.
See Page 2 for a full list of the status of Medicaid expansion and state exchanges for all 50 states, and the 2013 and midyear 2014 uninsured rates for each.
Implications
While a majority of Americans continue to disapprove of the Affordable Care Act, the uninsured rate is declining, as the law intended. Nationally, 17.3% of U.S. adults reported being without health insurance in 2013, a rate that had slowly increased from 14.8% in 2008. The uninsured rate peaked at 18.0% in the third quarter of 2013 -- the three months immediately preceding the opening of the healthcare exchanges -- and has since declined to 13.4% in the second quarter of 2014, the lowest quarterly rate in more than six years of Gallup-Healthways Well-Being Index trending.
At the state level, those that have implemented two of the law's core mechanisms -- Medicaid expansion and state health exchanges -- are seeing a substantially larger drop in the uninsured rate than states that did not take both of these actions. Consequently, the gap in uninsured that existed between the two groups in 2013 has now nearly doubled through the first half of 2014.
Many states continue to debate implementing these actions. New Hampshire recently became the 26th state (plus the District of Columbia) to expand Medicaid, which takes effect this summer. Utah, a conservative state with a Republican governor, Gary Herbert, continues negotiation with the Centers for Medicare and Medicaid Services to have revised, more flexible terms than what is detailed in the Affordable Care Act. Utah expanding Medicaid could serve as a blue print for other red states to follow, as could similar scenarios playing out in Indiana and Pennsylvania.
Other states, in turn, are debating dropping their state-based exchanges and moving to the federal exchange because of technological issues or unexpected cost-related challenges. Oregon will be designated as a supported state-based marketplace in 2015 that leverages federal technology, while Maryland is modifying its troubled website to model Connecticut's. Officials from the states of Massachusetts and Hawaii -- both of which had comparatively low uninsured rates to begin with but show little or no change since 2013 -- are also considering switching to the federal exchange, indicating that locally managed exchanges are not necessarily optimal for insurance sign-ups in some states.
Editor's note: This article originally asserted that Oregon was moving from a state-based exchange to the federal exchange. It has been updated to reflect that Oregon is moving to a supported state-based marketplace.
Survey Methods
Results are based on telephone interviews conducted as part of the Gallup-Healthways Well-Being Index survey Jan. 2-Dec. 29, 2013, with a random sample of 178,068 adults, aged 18 and older, living in all 50 U.S. states and the District of Columbia. A total of 88,678 respondents were interviewed Jan. 2-June 30, 2014.
The 2013 margin of sampling error for most states is ±1 to ±2 percentage points, but it is as high as ±3.5 points for states with smaller population sizes, such as Wyoming, North Dakota, South Dakota, Delaware, and Hawaii. For midyear 2014 results, the error range increases to as high as ±5.0 points for these smallest states.
Interviews are conducted with respondents on landline telephones and cellular phones, with interviews conducted in Spanish for respondents who are primarily Spanish-speaking. Each sample of national adults includes a minimum quota of 50% cellphone respondents and 50% landline respondents, with additional minimum quotas by time zone within region. Landline telephone and cellphone numbers are selected using random-digit-dial methods. Landline respondents are chosen at random within each household on the basis of which member had the most recent birthday.
Samples are weighted to correct for unequal selection probability, nonresponse, and double coverage of landline and cell users in the two sampling frames. They are also weighted to match the national demographics of gender, age, race, Hispanic ethnicity, education, region, population density, and phone status (cellphone only/landline only/both, cellphone mostly, and having an unlisted landline number). Demographic weighting targets are based on the most recent Current Population Survey figures for the aged 18 and older U.S. population. Phone status targets are based on the most recent National Health Interview Survey. Population density targets are based on the most recent U.S. census. All reported margins of sampling error include the computed design effects for weighting.
In addition to sampling error, question wording and practical difficulties in conducting surveys can introduce error or bias into the findings of public opinion polls.
For more details on Gallup's polling methodology, visit www.gallup.com.